Understanding Pain
Every 2 weeks here at Lattice, the coaches get together and take it in turns to lead a discussion on a topic of their choice. We use these sessions to further educate ourselves and share ideas on the wide range of topics that play into climbing and training for climbing. Here we are looking to share some of the main takeaways so that you can apply them to your own climbing and training!
This week coach Raf talked about Pain. Pain is something that unfortunately many climbers experience at some point in their training careers, and having a better understanding of it has been shown to lead to improved recovery from injury.
What is Pain and how does it work?
The way that the pain sensation is created is that you have these long, fast myelinated nerve fibres called nociceptors, and when they sense danger they will send danger signals to your spine. At this point there still isn’t any pain. Your spine continues this signal up to your thalamus, (still no pain) your thalamus then passes it on to your cerebral cortex, which is an area of the brain which is in charge of higher ordre functions such as sensation, perception, memory, association, thought, and voluntary physical action. Your brain will then do some really cool things by looking at your previous experience and knowledge and surroundings and many other factors to work out if you are in danger and whether a pain response is necessary.
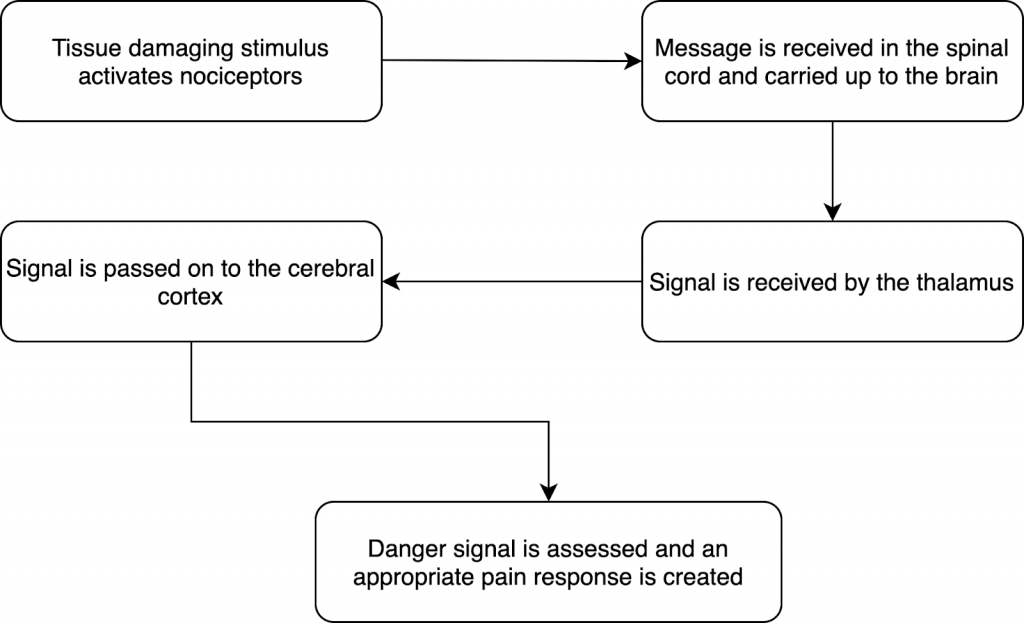
Pain is, in essence, a self defense mechanism which makes us react when we are in danger to help us to protect ourselves from causing further injury. It’s designed to make us react and seek “safety”. This is why it can often be the case that when you go to the doctor or physio, the thing that you went to see them about doesn’t hurt as much anymore. The reason for this is that the pain has already served its purpose in that it has gotten you to act and go seek professional help. Now that you are about to see your doctor or physio you feel safer – you perceive less danger, and there is less need to produce pain. As such, pain is a much more complex mechanism than “there is damage to my tissues therefore I am in pain” and there may be a biological, psychological and social contribution to how we experience pain.Pain is often an indicator that there is an injury, however there are many circumstances where there may be pain and no injury, or injury and no pain. So pain and injury certainly have a relationship, but they aren’t the same thing.
What does pain do and why is it useful to know about pain as a climber?
- This biopsychosocial model
The biopsychosocial model of pain is a widely accepted model of how pain works. The bio-logical part is what is actually happening in the body i.e. an injury or illness of some sort. The psycho-logical part of the equation is your beliefs and fears (what one person perceives as “danger”, another might perceive as “safe”), and the social part is the influence people around you have on how you experience pain or how they make you feel (think how you were brought up or whether or not you trust your doctor). The psychological and social parts of the biopsychosocial model make up two thirds of the model which shows that there is a huge amount that you can do to improve your pain experience outside of physical rehab.
“The brain produces pain when it weighs the world outside and in, and if it feels that there is more danger than safety. Likewise if your brain thinks that there is more safety than danger then there will be no pain.” Dr David Butler
- Understanding pain reduces the pain response
Interestingly there are numerous studies which demonstrate that understanding how pain works reduces the level of pain that is experienced, which in turn allows the rehabilitation process to proceed at a better rate or for people to perform their rehabilitation/start climbing with more confidence. The reason for this is that by understanding the process of how pain manifests you can reduce the fear surrounding that pain, and a reduction in fear reduces the “danger signals” coming from the ‘psycho’ part of the biopsychosocial model and reduces the need for pain production.
- Language
There are many things that will have an influence on whether we believe that there is danger and therefore need for pain. A good example of this is the type of language used around the injury. To help demonstrate this, have a think about which phrase sounds more scary and which you would prefer to hear from your doctor or physio.
- You’ve got a partial tear in your connective tissue.
- You’ve sprained your connective tissue.
The difference is small, but it frames the injury in a very different way which can have a big impact on the pain response. So be wary of scary sounding terms like rupture/slipped disk and the narrative you use when talking about any injuries you may have. There is obviously a balance to be struck here between respecting the severity of a given injury and not adding unnecessary stress. When injuries become chronic or have a long associated recovery there will be a long period of discussing the injury, and it is worth being aware of how ingrained certain narratives can become (this goes beyond what we call the injury, but how we talk about it and whether we are positive) and the impact this could have further down the line.
- Placebo
For a long time it wasn’t known what the placebo effect was or how it could be used, but as pain science has developed over the years a greater understanding of the placebo effect has evolved. There are countless studies which have looked at the placebo effect and pain with some fascinating results. When placebos are used to “treat” pain, patients see differing analgesic effects (reduction in pain response) depending not only on how they are administered, but what colour they are or even who they are administered by. For example we know that injecting an inert molecule (a placebo) is more effective than ingesting that same inert molecule. Capsules are more effective than tablets. Capsules that are transparent and have little red balls in them are better than opaque capsules and so on.
The effectiveness of a placebo will be enhanced if the person administering them has an eloquent manner of speaking, is more attractive, or if they have some expensive car keys laying on the table! Why? Because all of these things alter your subconscious perception about the effectiveness of your medical care. This will vary from person to person as our past experiences etc. will have an impact on how we perceive the world.

Why is this useful to know?
- Using the knowledge of the placebo effect in choosing your healthcare professional
Needless to say, many of us have been injured at one time or another, and we may be sidelined for longer than necessary due to the fear that surrounds our injury prolonging the pain we experience. Using what we know, the recommendation would be to see someone that your friends or coach trusts, and most importantly someone you trust (remember what plays into your psycho-social element may be different to a friend). Pushing your physio for an explanation of your injury and rehab that resonates with you and that you can understand is worthwhile. Some injuries may require a certain level of pain to be experienced during rehab, so understanding this and feeling reassured by your physio could have a positive impact on your recovery. The more we understand, the less that is unknown, and we generally fear the unknown! We recommend James Walker from the Sheffield Climbing Clinic.
- Accepting fear and moving forward
It’s important to remember when dealing with a new injury that fear is a natural part of the process, and this is where a knowledgeable and kind physio can not only help you to find an appropriate rehab plan, but they can also help to reframe your thoughts around the injury in a way that will be conducive to reducing your pain levels.

For some interesting links and resources check out;
Pain, the brain and your amazing protectometer
This is a great book which is worth reading on the topic of pain.
If you want a more in depth version of the book above you can read
I hope you enjoyed the second blog from our coaches educational series, look out for our next topic where we will be covering nutrition for females and those with female sex hormones.






